Table of Contents
Mechanism Of Urine Formation In Human:
Nitrogenous wastes are formed inside all the body cells. These wastes are transported to the kidneys by blood and are changed into urine by three processes-
- Ultrafiltration or Glomerular Filtration.
- Tubular Reabsorption or Selective Reabsorption.
- Tubular Secretion or Excretion or Augmentation.
Glomerular Filtration:
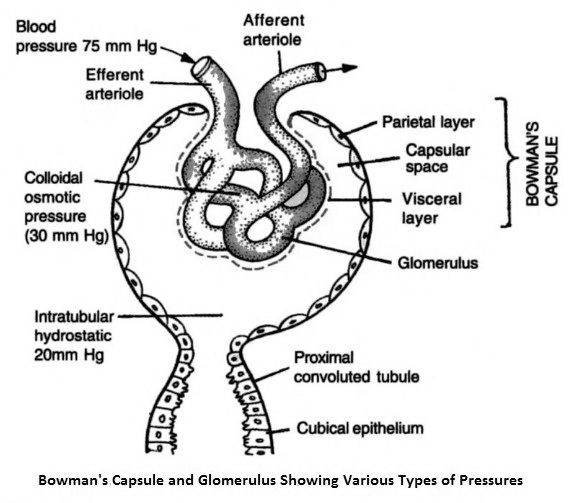
The first step in urine formation is the filtration of blood, which is carried out by the glomerulus and is called glomerular filtration which is a passive process. Blood enters the glomerulus through the afferent arteriole which has a wider diameter than the efferent arteriole that drains the blood. Therefore the blood pressure in the glomerular capillaries becomes very high so that there is a continuous process of filtration under pressure called ultrafiltration through glomerular capillaries. Blood enters the glomerulus at a hydrostatic pressure (HP) of 75 mm Hg in man which tends to filter out some fine components of blood but it is resisted by three pressures-
- The osmotic pressure (OP) of plasma proteins, especially albumin proteins in the glomerular capillaries is 30 mm Hg.
- The hydrostatic pressure of fluid present inside the renal tubule (HPN) is 10 mm Hg.
- The hydrostatic pressure of the interstitial fluid around the renal tubule (HPO) is 10 mm Hg.
So the net driving force which is responsible for ultrafiltration is provided by the difference between hydrostatic pressure at which blood enters glomerulus and the sum of opposing pressure and is called net filtration pressure or glomerular filtration pressure (GFP).
GFP = HP – (OP + HPN + HPO) = 75 – (30 + 10 + 10) = 25 mm Hg.
The filtered out fluid is known as Glomerular filtrate or Capsular filtrate or Nephric filtrate. Its composition is the same as blood minus cells and proteins. It resembles protein-free plasma in composition and osmotic pressure. It contains a large amount of water and other dissolved substances such as urea, uric acid, amino acids, creatinine, glucose, ammonia, sodium, potassium, vitamins, ketone bodies. Glomerular filtration rate (GFR) in a healthy individual is approximately 125 ml/minute, i.e., 180 litres per day.
Tubular Reabsorption:
From the Bowman’s capsule, the nephric filtrate enters the proximal convoluted tubule. This filtrate moves through the nephron towards the collecting duct by ciliary action. During its passage 99% of water, the whole of glucose, and amino acids most of Na+ and Cl-, some urea, and uric acid reabsorbed by peritubular capillaries. This process by which only useful substances are reabsorbed from the nephric filtrate in the blood capillaries is called selective reabsorption. It involves both passive and active transport across the tubular epithelium, chemically nephric filtrate is almost similar or isotonic to plasma.
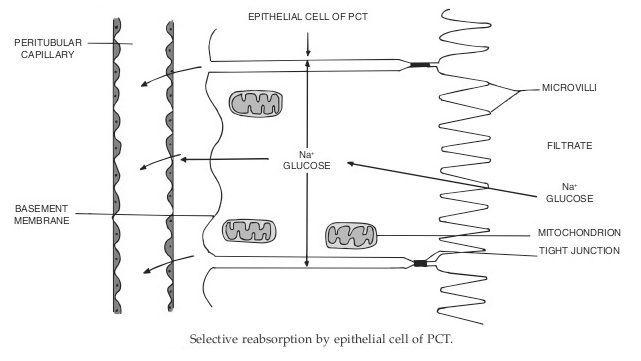
Proximal Convoluted Tubule (PCT) Reabsorption:
About 65% of the glomerular filtrate normally is reabsorbed before reaching the loops of Henle’s. Glucose and amino acids are specifically actively absorbed by secondary active transport from the glomerular filtrate into the blood capillaries. About 80% of filtrate water is passively absorbed by osmosis through the proximal tubular epithelium during reabsorption of solute. The tight junctions of PCT are often very loose and they allow rapid diffusion of water. About 70% of Na+, 75% of K+, and large amounts of Ca++ and almost all the vitamin C are absorbed here by the active transport process into the blood where sodium ions move into epithelial cells of proximal tubules along with carrier protein molecules and hydrogen ions are moved back in the opposite direction into tubular lumen by the same carrier protein molecule. This secretion of H+ ions by the tubular cells in exchange for Na+ (buffer bicarbonate- HCO3–) into tubular urine makes it acidic in nature. Urea and chloride ions are passively absorbed in the PCT. Urea molecule is very small and it is passively absorbed to some extent by diffusion along with water and the remaining urea passes out into the urine.
Reabsorption in Descending Limb of Henle’s Loop:
The anterior or first part of the descending limb is wider, thick-walled, which is connected with the PCT and is highly impermeable to the water, urea, and ions. The posterior part of the descending limb is narrow, thin-walled, highly permeable to water. Around this part of the descending limb hypertonic solution (NaCl, urea) is present in the interstitial fluid. Thus, water from the descending limb diffuses into the blood by exosmosis and drifted away by vasa recta. By the removal of water from the filtrate, glomerular filtrate becomes hypertonic.
Reabsorption in Ascending Limb of Henle’s Loop:
It is thick-walled, impermeable to water, however, the anterior narrow part of the ascending limb is highly permeable to NaCl and urea. NaCl leaves the ascending limb by diffusion into the surrounding interstitial fluids in the medullary regions. However, urea from the surrounding ISF enters the filtrate by the process of diffusion. From the posterior wider part of the ascending limb, Na+ and Cl– passes out by active transportation into interstitial fluids in the medullary regions. By the regular loss of Cl– and Na+, filtration becomes hypotonic to the blood plasma.
Reabsorption in Distal Convoluted Tubule (DCT):
The first half of the distal convoluted tubule is impermeable to water and urea and adds to the dilution of the tubular fluid. But the late distal convoluted tubule is permeable to water in the presence of the antidiuretic hormone (ADH) but impermeable when this hormone is absent. So, the additional osmotic removal of water occurs in the late distal convoluted tubule and filtrate becomes hypotonic. Besides this, there is active absorption of sodium ions (Na+) from the filtrate and this is controlled by the aldosterone hormone. The sodium ions finally pass into the peritubular interstitium but potassium and hydrogen are transported in the opposite direction into the tubular lumen. So, the distal convoluted tubule is a segment of selective secretion and reabsorption and also function in K+ and Na+ homeostasis.
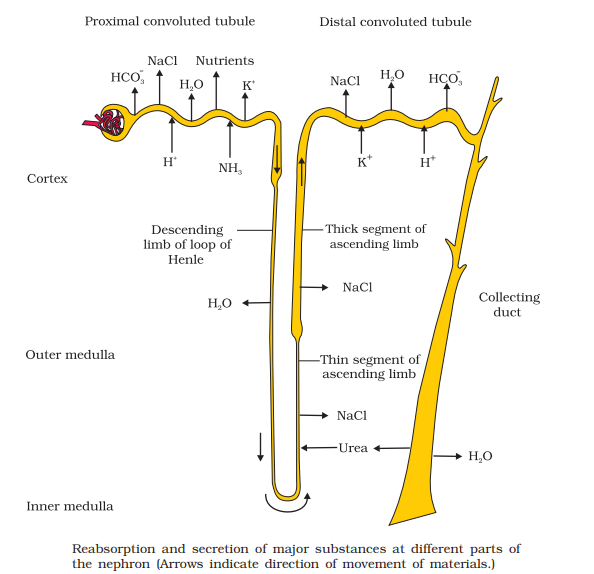
Reabsorption in Collecting Tubule and Collecting Duct:
The concentrated tubular fluid then enters the collecting tubule. The cuboidal epithelial cells of the collecting tubule are permeable to the water where an additional volume of water is absorbed osmotically from the tubular fluid and urine becomes hypertonic to the blood plasma. The filtrate then enters the collecting duct where the antidiuretic hormone of the posterior pituitary acts directly upon the epithelial cells of the collecting duct to increase the absorption of water into the medullary interstitium. The bottom portion of the collecting tubule is permeable to urea and leakage of this solute into interstitial fluid also adds to high osmolarity in medulla. This reduces the volume of urine and assists in concentrating the urine.
Tubular Secretion:
It is the process by which the glandular cells of nephrons, especially of DCT, excrete additional wastes like Uric acid, creatinine, hippuric acid, K+, H+, and NH3, etc., from the blood of particular capillaries into the filtrate by the process of active transport. Most of the K+ eliminated with urine is secreted by the cells of DCT and collecting tubules, in exchange for reabsorbed Na+.
Tubular secretion probably plays a minor role in human kidneys but it is the only mode of excretion in marine fishes and desert amphibians whose nephrons are without glomeruli and Bowman’s capsules.
As a result of these three processes, the wastes are changed into the urine. The volume of urine is much less as compared to the nephric filtrate due to the loss and gain of substances in the tubule. So urine is the glomerular filtrate reaching the end of the collecting duct, after reabsorption and additions of other substances.









Comments (No)