Table of Contents
Male Reproductive System:
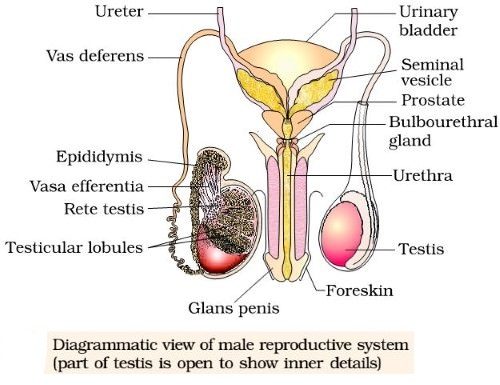
The male reproductive system is composed of testes together with accessory ducts and structures including the epididymis, vas deferens, ejaculatory duct, the distal portion of the urethra, the penis and several glands.
Testes:
Man possesses two ovoid glandular testes which are concerned with the formation of male gametes, the spermatozoa. Testes are suspended in thin pouches of skin and connective tissue, called scrotal sacs located outside the main body cavity behind the penis. Consequently, the testes exist at a temperature of 2 to 3°C lower than that of the rest of the body, which is favourable for sperm production. Each testis is encased in a capsule of white fibrous connective tissue, called tunica albuginea. Inside each testis are about 250 lobes or lobules, each of which contains one to three seminiferous tubules which are highly coiled structures involved in the formation of spermatozoa. Between the seminiferous tubules are found clumps of interstitial cells (or cells of Leydig) which secrete male sex hormone, the testosterone (an androgen). Testosterone regulates the development and maintenance of primary and secondary male characteristics and formation of spermatozoa.
Epididymis:
The seminiferous tubules of the testes open into the vas efferentia which after leaving the testes become confluent and form a folded tubular compressed mass of connective tissue called as epididymis. It lies along the inner side of each testis and constitutes the body and tail. The epididymal duct is thickened and leaves the tail of the epididymis as vas deferens. Epididymis stores the sperms temporarily until they become matured.
Vasa Deferentia or Vas Deferens:
A pair of thick-walled and muscular tubes, each of 35 to 40 cm develop from cauda epididymis. Vas deferens is initially coiled. It becomes straight and enters the abdominal cavity through the inguinal canal. It passes over urinary bladder and receives a pair of seminal vesicles. End of vas deferens is a little bit enlarged to form Ampulla for the storage of sperms. Vas deferens is internally lined by stereocilia for the conduction of sperms.
Urethra:
It arises from the urinary bladder and is about 20 cm long. The male urethra is differentiated into four parts-
- Urinary Urethra- It is the first part of the urethra which receives urinary bladder and carries urine only.
- Prostatic Urethra- Urethra is surrounded by prostate glands and here it also receives secretions from a pair of Cowper’s gland.
- Membranous Urethra- This part of the urethra is not covered by any covering.
- Penile Urethra- It is posterior most, the longest part of the urethra that passes through copulatory organ or penis and open at the tip of the penis.
Urethra has two sphincters:
- Internal Sphincter- It is composed of smooth muscles which are involuntary in nature.
- External Sphincter- It is composed of striated muscles which are voluntary in nature.
The urethra is a common passage of urine and genital discharge (semen). It is also called the urinogenital tract. Its opening is called the urinogenital aperture.
Penis:
It forms the external male genital organ. The urethra passes through its centre and makes a common passage for the exit of urine and semen. Around the urethra, there are three columns of spongy, erectile tissues (two corpora cavernosa and one corpus of spongiosum) that fill with blood to cause the penis to become erect and hard. Externally penis is covered by skin. At the distal end of the penis, there is a slight bulging and highly sensitive structure called the glans penis which is partially covered by a thin fold of skin, the foreskin or prepuce.
Accessory Glands:
Seminal Vesicles:
These are paired, a tubular, club-shaped structure situated just above the prostate gland and near the base of the urinary bladder and at the interior of the rectum. The ducts from the seminal vesicles join the posterior part of vas deferens and form the common ejaculatory duct. The seminal vesicles secrete clear alkaline, yellowish, viscous fluid and contain globulin, citrate, inositol fructose and flavins. Fructose provides energy to facilitate the motility of sperms after ejaculation and flavin give semen a strong fluorescence in UV light. The secretions of seminal vesicles constitute about 60-70% part of the ejaculate.
Prostate Gland:
It is a large pyramidal, chestnut shaped gland that encloses a part of urethra including its junction with the ejaculatory ducts. The prostate gland contains 30-40 alveoli which open separately into urethra by fine ducts. Secretions of the prostate gland are thick, milky and alkaline, constituting up to 20-30% of semen. It is essential for sperm motility (removal causes sterility), activate sperm.
Cowper’s or Bulbourethral Glands:
These glands are located slightly below the prostate gland, on either side of the urethra. They are about the size of pea seed and form the floor of the pelvis. They secrete, clear, white, a viscous, alkaline, mucoid lubricant that neutralizes the activity of acidic female vaginal secretions and increases the mobility and survival potentiality of sperms in the genital tract of a female.
Semen:
Sperms are quite immotile when first produced; they pass into the epididymis where they are stored. They are activated and made motile by the secretions from the accessory reproductive organs. These secretions are collectively designated as seminal fluid or seminal plasma and are added to the spermatozoa during ejaculation. The seminal plasma along with the spermatozoa forms the semen. The alkalinity (pH 7.3 – 7.5) of the seminal fluids is maintained by the prostate and Cowper’s glands and it protects the spermatozoa from the fatal acidity present in the male urethra and female genital tract. A single ejaculate consists of 200 to 600 millions of spermatozoa in 4 to 5 ml of semen.
FSH (Follicle-stimulating hormone) and LH (Luteinizing hormone) from anterior pituitary gland regulate the growth and functioning of the seminiferous tubules and Leydig cells respectively. Leydig cells secrete testosterone which regulates the functioning of secondary sex organs.
- Differences Between Spermatogenesis And Oogenesis
- Passive and Active Absorption of Food
- Alimentary Canal of Man
- Differences Between Algae And Fungi
- Essential and Non-essential Parts of the Flowers
- Pollination: Types and Its Importance
- Enzymes And Their Properties
- Constituents of Food: Carbohydrates, Proteins, Fats & Vitamins
- Nutrition and Digestion-NIOS









Comments (No)